Equine gastric ulcers are all too common, affecting up to 93% of horses. Ulcers are painful lesions that form in the lining of the gastrointestinal tract that can result in impaired nutrient absorption, discomfort, digestive complications, and poor performance in your horse.
Traditionally, veterinarians and horse owners treated and managed all gastric ulcers the same way. However, their etiology and physiology differs depending on the region of the stomach in which they appear. [1][5]
- Equine Squamous Gastric Ulcer Syndrome (ESGUS) refers to ulcers affecting the upper squamous region of the stomach.
- Equine Glandular Gastric Ulcer Syndrome (EGGUS) refers to ulcers affecting the lower glandular region of the stomach.
What’s the difference between squamous ulcers and glandular ulcers in horses?
Research shows that there are different risk factors and causes for squamous ulcers compared to glandular ulcers. There are also different treatment and management strategies recommended for EGGUS vs. ESGUS.
Understanding the differences between these two ulcer syndromes can help you identify, prevent, and manage gastric ulcers in your horse.
Overview of Gastric Ulcers
Equine gastric ulcers are sores or lesions in the lining of the stomach. They are one of the most commonly diagnosed health conditions in horses.
Horses are usually diagnosed with the umbrella term Equine Gastric Ulcer Syndrome (EGUS). This diagnosis can include ulcers of the squamous region and ulcers of the glandular area.
Ulcers that appear in the upper squamous region are more common than those that develop in the lower glandular region, largely due to the different natural defence systems these two regions have against ulcers.
Below, we will review further differences in risk factors, causation, diagnosis, treatment, and prevention of squamous versus glandular ulcers. [1]
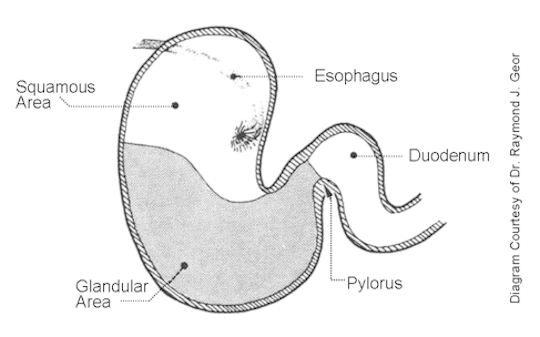
Equine Squamous Gastric Ulcer Syndrome (ESGUS)
Up to 80% of all equine ulcers are found in the squamous region of the stomach, which is the upper one-third of the stomach. [2] The causes and risk factors for ESGUS are well understood.
The stomach is a harsh environment. Stomach acid (HCl) has a very low pH, making it corrosive and potentially damaging to the cells that line the inside of the stomach. This mucosal layer on the inside of the stomach is made up of epithelial cells.
HCl is continuously secreted from acid-producing cells in the glandular region of the stomach. Therefore, the epithelial cells of the glandular region are well adapted to constant contact with stomach acid and have two distinct defense mechanisms to protect themselves from degradation and damage:
- The production of mucous, which coats the glandular epithelium.
- The production of bicarbonate, which buffers stomach acid coming into direct contact with the stomach wall
Conversely, the epithelial cells of the squamous region of the stomach lack these defense mechanisms. This is because these cells are not routinely exposed to stomach acid for long durations. This is why ESGUS is significantly more prevalent than EGGUS. [3]
The squamous epithelium can be over-exposed to gastric acids when the stomach is empty for extended periods of time or when acid splashes up onto the squamous region, particularly during exercise.
Consumption of feed actually helps to prevent some of the damage caused by gastric acids in the squamous lining. Food, saliva, and water all work to buffer some of these acids. Feeding your horse many small meals throughout the day can help to reduce ulcer risk.
Equine Glandular Gastric Ulcer Syndrome (EGGUS)
Compared to squamous ulcers, much less is known about EGGUS and the pathophysiology of this disease.
The glandular region comprises the bottom two-thirds of the stomach. [2] This region is where acid secretion takes place.
The major gastric acid secreted is hydrochloric acid (HCl). Pepsin and gastrin are also secreted in this region. These acids activate digestive enzymes to begin the breakdown of food.
As discussed previously, the glandular region produces bicarbonate and mucous. These compounds buffer gastric juices and line the stomach wall of the glandular region protecting it from acid damage.
Therefore, acid damage is not usually the cause of EGGUS. Rather, it appears that interference with these defense mechanisms and disruption of mucosal integrity are the causes of ulcers in this region. [3]

Gastric Ulcer Prevalence in Horses
Equine ulcers are extremely common, but the prevalence is much higher for ESGUS compared to EGGUS.
Prevalence depends on lifestyle, diet, and environmental factors. It varies considerably between squamous and glandular ulcers.
Prevalence of ESGUS
For squamous ulcers, the prevalence appears highest in racing and performance horses. Specifically, Thoroughbred racehorses have the highest prevalence.
Untrained Thoroughbred horses have an estimated prevalence of 37%. Thoroughbred horses in training for more than 2 months have reported prevalence between 80-100%. [11][12][13]
Standardbred racehorses have a similar but slightly lower prevalence of ESGUS. Only a 44% prevalence is reported in untrained Standardbred horses but up to 87% of training Standardbred racehorses are affected by squamous ulcers. [14][15]
Forty-eight percent of non-competing endurance horses are affected by ESGUS. [8] This prevalence increases to 93% when competing. [16]
Furthermore, up to 58% of both show and pleasure horses are affected by ESGUS. [17][18]
Prevalence of EGGUS
There is limited research on the prevalence of EGGUS in horses. Up to 65% of Thoroughbred racehorses may be affected by EGGUS. [6]
Competing endurance horses are thought to have a prevalence of between 27-33%. The prevalence of glandular ulcers is approximately 16% when not competing. [7][8]
Preliminary data suggests that Warmblood horses are most likely to be affected by EGGUS. [9] However, only one study has shown this association when compared to other horse breeds.
The prevalence of EGGUS in show horses is unclear. Up to 54% of pleasure horses are reported to be affected by EGGUS. [10]
Risk Factors for ESGUS and EGGUS
Current research on risk factors for equine ulcers tends to focus on EGUS as a whole. As new findings emerge, they show there are clear differences between the risk profiles for ESGUS and EGGUS.
The risk of squamous ulcers is related to increased exposure to damaging acids along the stomach lining. [3][4]
The development of glandular ulcers involves impaired defense mechanisms such that the protective barrier of the stomach is weakened. [3][4]
Risk Factors for Squamous Ulcers
Common risk factors for ESGUS include: [3][4][5]
- High-intensity training
- High grain or concentrate intake
- Restricted forage intake or reliance on meal-feeding
- Limited turnout
- Changes to the social environment
- Lack of routine
- Travel and competition
Risk Factors for Glandular Ulcers
Risk factors for EGGUS include factors that weaken or lessen the integrity of the protective functions in the glandular region.
Research shows that the following are correlated with an increased risk of EGGUS: [3][4][5]
- Long-term use of non-steroidal anti-inflammatory drugs (NSAIDs)
- Limited turnout
- Short, intense exercise
- Breed (i.e. Warmblood)
- Presence of pathogenic bacteria
- Low hay intake
- High unprocessed grain intake
- Feeding an incomplete or unbalanced diet
Diagnosing Gastric Ulcers
To formally diagnose equine ulcers, a veterinarian will perform a gastroscopic exam.
This procedure is routinely performed under standing sedation after a period of fasting so that the stomach is empty. The gastroscope is a 3-meter-long flexible tube with a camera inside. It is passed through your horse’s nostril, down the esophagus, and into their stomach.
Your veterinarian will be able to visualize the esophagus, stomach, and most proximal portion of small intestine (duodenum). Your vet will assess the number and severity of ulcers present, as well as identify which area is affected (i.e. squamous or glandular region).
Gastroscopy is the only definitive way to diagnose gastric ulcers. Unfortunately, it can be expensive and is not always accessible to all horse owners. Due to the high prevalence of ulcers, it is common practice to assume that a horse is affected by this condition if they display certain characteristic signs or symptoms.
However, it is important to remember that squamous ulcers and glandular ulcers are treated differently. Treatment is also costly and time-consuming, which is why a definitive diagnosis via gastroscopy is important.
Grading Ulcers
To describe the severity of your horse’s gastric ulcers, your veterinarian will assign them a grade or score. At present, there is only a standardized grading system for squamous ulcers. [3]
Any score assigned to glandular ulcers should be accompanied by a detailed description since no grading rubric has been established yet. Lesions can be described by their number, distribution, appearance, and subjective degree of severity. [3]
| Grade/Score | Squamous Ulcers |
|---|---|
| 0 | Epithelium is intact. No appearance of hyperkeratosis (thickening of the mucosa). |
| 1 | Mucosa is intact. Areas of hyperkeratosis. |
| 2 | Small, single, or multifocal superficial lesions (less than 5) |
| 3 | Large, single deep, or multifocal superficial lesions (greater than 5) |
| 4 | Extensive lesions. Areas of apparent deep ulceration. |
Signs & Symptoms of ESGUS & EGGUS
There are many differences between ESGUS and EGGUS. However, the signs and symptoms are relatively similar.
Nonetheless, it’s important to note that every horse presents differently when it comes to gastric ulcers. The severity of clinical signs does not always correlate with the severity of ulcers diagnosed via gastroscopy – some horses are more stoic and others more dramatic when it comes to expressing discomfort.
If your horse exhibits any of the following signs and symptoms of equine ulcers, contact your veterinarian: [3][4][5]
- Poor appetite or picky eating
- Chronic diarrhea
- Weight loss and/or poor body condition
- Stretching to urinate
- Increased aggression or irritability
- Poor performance or behavior changes under saddle
- Poor hair/coat condition
- Recurrent colic
- Behavioural changes (ie. anxiety)
- Sensitivity in the girth area (girthiness)
- Cribbing, teeth grinding, and other stereotypic behaviours
- Excessive salivation
- Excessive recumbency (lying down)
Treatment of ESGUS & EGGUS
After a diagnosis, your veterinarian will develop the best treatment plan for your horse. Strategies to treat ulcers differ between ESGUS and EGGUS.
Treatments for ESGUS
1. Omeprazole
This drug is a proton pump inhibitor. It irreversibly blocks the production of gastric acid to increase the pH level (reduce acidity) in the stomach.
In the stomach, proton pumps use an enzyme to trade hydrogen ions for potassium ions. Once absorbed, omeprazole binds to this enzyme and prevents the pump from working properly, which decreases hydrogen chloride production. [19]
Veterinarians often prescribe omeprazole treatment to horses with ESGUS. It is the only FDA-approved drug for the treatment of equine gastric ulcers, sold under the tradenames GastroGard or UlcerGard.
Omeprazole is administered orally once a day at a dose of 4 mg/kg body weight (2000 mg omeprazole for a 500 kg horse). [20] The treatment course is typically long, lasting four weeks or 28 days.
2. Ranitidine and Cimetidine
These two drugs are histamine H2 receptor blockers that also reduce the production of gastric acid. These options are often cheaper than omeprazole.
However, studies show that ranitidine and cimetidine are less effective at treating ulcers than omeprazole. [21]
3. Antacids
Antacids have long been used to treat gastric ulcers. They neutralize gastric acids instead of inhibiting their production. [22]
Antacids have been shown to increase the stomach pH levels in horses for short durations (2 – 4 hours maximum). [23]
They are less likely to be recommended due to their temporary efficacy and potential adverse effects on digestion. [24]
Treatments for EGGUS
1. Misoprostol
Misoprostol is a synthetic prostaglandin, which is a type of immune compound that inhibits acid secretion and stimulates mucous secretion in the glandular stomach.
As a prostaglandin analogue, misoprostol may improve glandular mucous barrier function and integrity.
Research shows that horses treated with misoprostol exhibit increased mucous and bicarbonate production. Additionally, misoprostol has shown anti-inflammatory effects. [25]
One clinical trial in horses with glandular ulcers showed that misoprostol treatment was more effective than omeprazole. [26]
2. Sucralfate
Sucralfate is a mucosal protectant. It forms a physical barrier to protect the gastric mucousa against degradation by gastric acids. This helps facilitate ulcer healing and decreases pain associated with ulcers. [27]
Administration of sucralfate in horses also improves the secretion of mucous and bicarbonate. This can provide further protection for the stomach lining.
Sucralfate is often administered alongside other treatment options such as omeprazole to increase its efficacy. Timing of administration and your horse’s feeding schedule needs to be carefully managed so as to not impair absorption. [3]
3. Omeprazole
Treatment for EGGUS may also include omeprazole. However, studies show that omeprazole is only 25% effective at treating ulcers in the glandular region. [6]
Prevention and Management of Ulcers
There are many changes you can adopt in your horse’s feeding and management to prevent gastric ulcers.
Some strategies work to prevent both ESGUS and EGGUS. However, specific strategies may be better for squamous ulcers while other strategies target glandular ulcers.
Lifestyle Strategies
Incorporating some of the following changes in your horse’s daily routine can naturally reduce ulcer risk.
- Avoid intermittent feeding
- Provide constant access to water
- Increase turnout
- Reduce grain consumption
- Increase haylage and hay quality
- Minimize NSAID use
- Provide your horse with a suitable social group
Feeding Strategies
Certain hays are known to reduce ulcer risk, such as protein-rich alfalfa hay. Feeding supplemental oils to reduce grain consumption can also decrease risk factors for a number of gut problems.
It’s also important to ensure you are providing your horse with free-choice loose salt and adding 1-2 tablespoons of salt per day to your horse’s ration.
Salt consumption helps to encourage water intake, which can help to buffer against gastric acids. Hydration also promotes the transit of food through the gastrointestinal tract.
Several safe and natural nutritional supplements have also shown benefits for gastric ulcers.
Ulcer supplements may work by supporting gut barrier function, promoting overall digestive health or by supporting tissue repair.
Some ingredients that have research-based evidence to support their use include:
- Pectin-Lecithin complex: Exerts a mucous protective effect that may be beneficial for both squamous and glandular ulcers [28][29]
- Yeast: A probiotic that may help reduce the risk of squamous ulcers [30]
- Amino Acids: (i.e. glycine, glutamine) Involved in the building and repair of tissues in the stomach lining [31][32]
- Sea buckthorn berry extract: Its high antioxidant content may be beneficial for EGGUS [33]
Visceral+
Mad Barn’s Visceral+ is a pelleted supplement that provides nutritional support for your horse’s digestive system, including support stomach health and the hindgut.
Discuss any feeding program changes with our qualified equine nutritionists. You can submit your horse’s diet for individualized recommendations.
If you think your horse has squamous or glandular ulcers, please contact your veterinarian to decide on the best treatment plan.
References
- Sykes, B.W. and Jokisalo, J.M. Rethinking equine gastric ulcer syndrome: Part 1 – Terminology, clinical signs and diagnosis. Equine Vet Edu. 2014.
- Geor, R.J. et al. Equine Applied and Clinical Nutrition. 2013.
- Sykes, B.W. et al. European College of Equine Internal Medicine Consensus Statement—Equine Gastric Ulcer Syndrome in Adult Horses. J Vet Intern Med. 2015. View Summary
- Sykes, B.W. and Jokisalo, J.M. Rethinking equine gastric ulcer syndrome: Part 3 – Equine glandular gastric ulcer syndrome (EGGUS). Equine Vet Edu. 2015.
- Sykes, B.W. et al. Management factors and clinical implications of glandular and squamous gastric disease in horses. J Vet Intern Med. 2018. View Summary
- Sykes B.W. et al. A comparison of three doses of omeprazole in the treatment of equine gastric ulcer syndrome: A blinded, randomised, dose-response clinical trial. Equine Vet J. 2014. View Summary
- Tamzali, Y. et al. Prevalence of gastric ulcer syndrome in high-level endurance horses. Equine Vet J. 2014. View Summary
- Nieto, J.E. et al. Prevalence of gastric ulcers in endurance horses–a preliminary report. Vet J. 2004. View Summary
- Monki, J. et al. Risk Factors for Equine Gastric Glandular Disease: A Case‐Control Study in a Finnish Referral Hospital Population. J Vet Intern Med. 2016. View Summary
- Hepburn, R.J. Endoscopic examination of the squamous and glandular gastric mucosa in sport and leisure horses: 684 horses (2005–2011) [abstract”] Proc 11th International Equine Colic Research Symposium. 2014.
- Murray, M.J. et al. Factors associated with gastric lesions in thoroughbred racehorses. Equine Vet J. 1996. View Summary
- Begg, L.M. and O’Sullivan, C.B. The prevalence and distribution of gastric ulceration in 345 racehorses. Aust Vet J. 2003. View Summary
- Vatistas, N.J. et al. Cross-sectional study of gastric ulcers of the squamous mucosa in thoroughbred racehorses. Equine Vet J Suppl. 1999. View Summary
- Dionne, R.M et al. Gastric ulcers in standardbred racehorses: prevalence, lesion description, and risk factors. J Vet Intern Med. 2003. View Summary
- Rabuffo, T.S. et al. Associations between age or sex and prevalence of gastric ulceration in Standardbred racehorses in training. J Am Vet Med Assoc. 2002. View Summary
- Tamzali, Y. et al. Prevalence of gastric ulcer syndrome in high-level endurance horses. Equine Vet J. 2011. View Summary
- McClure S.R. et al. Prevalence of gastric ulcers in show horses. J Am Vet Med Assoc. 1999. View Summary
- Luthersson N. et al. The prevalence and anatomical distribution of equine gastric ulceration syndrome (EGUS) in 201 horses in Denmark. Equine Vet J. 2009. View Summary
- Fellenius E. et al. Substituted benzimidazoles inhibit gastric acid secretion by blocking (H+ + K+)ATPase. Nature. 1981.
- Merial Inc. GastroGard – Omeprazol paste. 2018.
- Lester G.D. et al. Effects of treatment with omeprazole or ranitidine on gastric squamous ulceration in racing Thoroughbreds. J Am Vet Med Assoc. 2005. View Summary
- Salisbury B.H. & Terrell J.M. Antacids. StatPearls Publishing. 2020.
- Murray M.J. Grodinsky C. The effects of famotidine, rantidine and magnesium hydroxide/aluminium hydroxide on gastric fluid pH in adult horses. Equine Vet J Suppl. 1992. View Summary
- Hade J.E. and Spiro H.M. Calcium and acid rebound: a reappraisal. J Clin Gastroenterol. 1992.
- Wallace J.L. Prostaglandins, NSAIDs, and gastric mucosal protection: why doesn’t the stomach digest itself?. Physiol Rev. 2008.
- Varely G. et al. Misoprostol is superior to combined omeprazole-sucralfate for the treatment of equine gastric glandular disease. Equine Vet J. 2019. View Summary
- Rees W.D. Mechanisms of gastroduodenal protection by sucralfate. Am J Med. 1991.
- Venner M. et al. Treatment of gastric lesions in horses with pectin-lecithin complex. Equine Vet J Suppl. 1999. View Summary
- Ferrucci F. et al. Treatment of gastric ulceration in 10 standardbred racehorses with a pectin-lecithin complex. Vet Rec. 2003. View Summary
- Sykes B.W. et al. Efficacy of a Combination of Apolectol, Live Yeast (Saccharomyces cerevisiae [CNCM I-1077]), and Magnesium Hydroxide in the Management of Equine Gastric Ulcer Syndrome in Thoroughbred Racehorses: A Blinded, Randomized, Placebo-Controlled Clinical Trial. J Equine Vet Sci. 2014.
- Wang W. et al. Glycine metabolism in animals and humans: implications for nutrition and health. J Amino Acids, 2013.
- Rotting A.K. et al. Effects of phenylbutazone, indomethacin, prostaglandin E2, butyrate, and glutamine on restitution of oxidant-injured right dorsal colon of horses in vitro.. Am J Vet Res, 2004. View Summary
- Huff N.K. et al. Effect of Sea Buckthorn Berries and Pulp in a Liquid Emulsion on Gastric Ulcer Scores and Gastric Juice pH in Horses. J Vet Intern Med. 2012. View Summary













Leave A Comment